To The Teacher
Vaccines for Covid-19 have been approved for emergency use in a variety of countries, including the United States. This news potentially signals a coming end to the pandemic. But a program of mass vaccination raises some tricky political issues: Who will be first in line to receive the vaccine? Will people trust the public health agencies carrying out the vaccinations? And will the distribution of the vaccine address the systemic inequities that have led to Covid disproportionately impacting communities of color?
This lesson includes two readings that will explore the politics of vaccines and vaccinations. The first reading examines some fears about vaccines, including ones based in misinformation as well as others that reflect the history of racism in public health. The second reading considers the question of what groups will be prioritized for vaccinations and how decisions about who goes first are made. Questions for discussion follow each reading. Pdf versions of the readings are here.
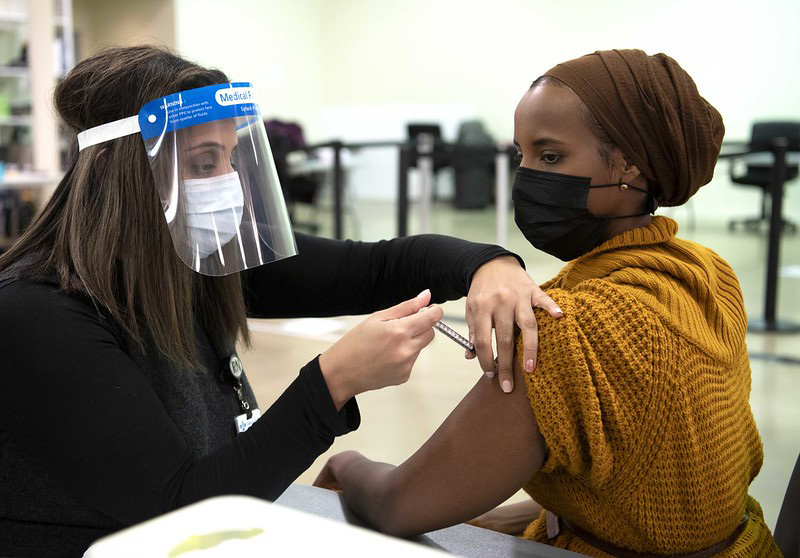
Reading One
Addressing Concerns About Vaccination
pdf version
Vaccines for Covid-19 have been approved for emergency use in a variety of countries, including the United States. This news potentially signals a coming end to the pandemic. Of course, there’s more to a vaccine than its development and approval. Supplies of a vaccine must be delivered in sufficient quantities to cover a population, and large numbers of people must actually get vaccinated.
In a poll released on December 15, 2020, the Kaiser Family Foundation found that the number of Americans who plan to get a Covid vaccine when it becomes available has increased in recent weeks. About 71 percent of respondents said they would get a vaccine, up from 63 percent in an August/September poll. The increase was evident across all racial and ethnic groups surveyed, as well as both Democrats and Republicans. Confidence has grown as more and more people have been vaccinated – including political leaders such as President-elect Joe Biden, Vice President-elect Kamala Harris, and Vice President Mike Pence.
However, just over a quarter of those polled were still skeptical, saying that they probably or definitely would not get vaccinated, even if the vaccine is available for free and determined by scientists to be safe.
According to New York Institute of Technology assistant professor Jonathan Berman, author of Anti-vaxxers: How to Challenge a Misinformed Movement, some vaccine skeptics are “people who have reservations about being vaccinated, but are still open to being assured that the treatments are safe and reliable.” But there are also “anti-vaxxers,” a “more concrete, organized movement of people who actively try [to] suppress vaccination as a [practice] and prevent people from getting vaccinated, and their minds are far harder to change….”
According to Berman, for anti-vaxxers, “The arguments don’t matter. They have this fear of vaccines that’s driven by emotion and stories their neighbors and friends have told them, which they use to justify those beliefs.” Anti-vaxxers often cite bogus studies and debunked theories about the hazards of vaccines.
To build public trust, those who have studied the “anti-vaxx” movement, like Berman, recommend making peer-reviewed scientific studies available to the public and allowing journalists to examine the inner workings of vaccine trials so that they can better communicate the safeguards that have been used. (Studies that have been “peer-reviewed” have been evaluated by other experts in the relevant field.)
Apart from the anti-vaccination movement, other groups may have concerns about the Covid-19 vaccine that are rooted in historical realities. As New York Times columnist Charles Blow explained in a December 6, 2020 column, African-Americans as a group have expressed a greater level of skepticism about vaccination, owing in part to patterns of racism in American medical history. Blow writes:
It would appear that the people in America hit hardest by Covid-19 — Black people — are also the group most leery about the prospects of a vaccine.
As a Pew Research report published last week pointed out: “Black Americans are especially likely to say they know someone who has been hospitalized or died as a result of having the coronavirus: 71 percent say this, compared with smaller shares of Hispanic (61 percent), White (49 percent) and Asian-American (48 percent) adults.”
But that same report contained the following: “Black Americans continue to stand out as less inclined to get vaccinated than other racial and ethnic groups ….
The unfortunate American fact is that Black people in this country have been well-trained, over centuries, to distrust both the government and the medical establishment on the issue of health care.
In the mid-1800s a man in Alabama named James Marion Sims gained national renown as a doctor after performing medical experiments on enslaved women, who by definition of their position in society could not provide informed consent….
Furthermore, as the Centers for Disease Control and Prevention explains: “In 1932, the Public Health Service, working with the Tuskegee Institute, began a study to record the natural history of syphilis in hopes of justifying treatment programs for Blacks… Hundreds of Black men were told they were being treated for syphilis, but they were not. They were being observed to see how the disease would progress. The men suffered under this experiment for 40 years….
I hope that America can overcome Black people’s trepidations about this vaccine, but it is impossible to say that that trepidation doesn’t have historical merit.
Given this horrific history, Dr. Ala Stanford, a surgeon and founder of the Black Doctors Covid Consortium, told the Philadelphia Inquirer: “I think we have to stop saying that ‘Black people don’t trust the healthcare system.’ It is that the healthcare system has been untrustworthy to African Americans. There’s a difference and that’s the history.”
However, the evidence for the safety and efficacy of the Covid vaccine is strong. Dr. Stanford and her consortium plan to work to ensure that Black Philadelphians get vaccinated. The Inquirer reported, “Last spring, [Dr.] Stanford began administering Covid tests in church parking lots and going to people’s homes because too many African Americans had been going without. She and the doctors who joined her filled an important void. They plan to do the same when it comes to getting [people] vaccinated.”
In the coming months, public officials will be working to build trust and ensure that a vaccine can truly put an end to a pandemic that has caused such disproportionate suffering in Black and brown communities.
For Discussion:
- How much of the material in this reading was new to you, and how much was already familiar? Do you have any questions about what you read?
- According to the reading, what is the “anti-vaxx” movement?
- What are some ways that public health officials are working to combat the misinformation spread by this movement?
- New York Times columnist Charles Blow argues that African-Americans have reasons to be more wary of vaccination programs due to a history of racism in American medicine. What are some past incidents that may have contributed to this distrust?
- Given concerns about vaccination—ranging from fears based on misinformation to those more rooted in American history—how would you suggest that public officials build trust for a vaccination program? What information might you include if you were in charge of a public awareness campaign encouraging people to get the Covid vaccine?
Reading Two
Who Will Get the Vaccine First? Politics, Race, Students, and Prisons
As vaccines for Covid-19 have started to be approved for emergency use, an important question has emerged: Who should get it first?
There is widespread agreement that frontline medical professionals and those working in nursing homes should be vaccinated as quickly as possible. But after that, the question of priority becomes a debate.
Many believe that other workers who do essential work– such as food workers, manufacturing workers, transit workers, and teachers – should be high on the list, since they are putting their lives at risk to do work that sustains the rest of us. As Kareem Abdul-Jabbar points out in an article for WebMD, a high percentage of these essential workers are people of color. He notes that “one of the reasons Blacks are contracting and dying from Covid-19 at higher rates is because they work at what the government has defined as essential jobs more than any other ethnic group: 37.7% Black versus 26.9% white. In health care and social assistance industries, the rate is even higher.”
But although communities of color have been disproportionately affected by the pandemic, it is not clear whether government guidelines will make provisions to prioritize these communities.
Students and other young people are far less likely to die from Covid than their grandparents, but some have argued that vaccinating young people early can nevertheless be desirable—both because of the societal need to reopen schools and because targeting younger adults could be a more effective means of ending the pandemic if these groups are the ones most likely to spread the virus.
In a November 27, Politico reporters Ryan Heath and Carmen Paun discussed some of the considerations that public officials are debating as they determine who will be first to receive the vaccine. They wrote:
Many disputes over prioritization will play out in the fine print of government plans. Is a hospital janitor more at risk than a suburban pediatrician? Is a truck driver’s super-spreading danger a greater priority than the risk faced by a 50-year old with diabetes?
“You want to target the highest risk, because this will get you the biggest benefit,” said Tom Kenyon, a former director of CDC’s Center for Global Health, now chief health officer at the non-profit Project HOPE, who cited the example of truck drivers in Africa being identified as key spreaders of the virus….
While federal and state officials agree that the nation’s 21 million health care workers should be first in line for the vaccine, there is no consensus about how to balance the needs of other high-risk groups. [Secretary of Health and Human Services Alex] Azar said this week that states will have the "final say" in prioritizing Covid vaccinations, and that the shots will be apportioned according to the size of adult populations…
California Gov. Gavin Newsom pledged that hard-hit “Black and brown communities disproportionately are benefited” in California’s prioritization plan.
Moncef Slaoui, the former GlaxoSmithKline executive who leads Operation Warp Speed, said there are no easy choices.
"I don’t expect the states to make uniform decisions,” he told Politico. “Some may prefer long-term care facilities or the elderly, while others may prioritize their health care workers. It would be wrong to immunize 18-year-olds first. I hope no one does that. But otherwise it’s shades of gray.”
While we might hope that decisions on vaccination priorities are based on who needs the vaccine most, in reality political biases may come into play, leaving some groups unfairly neglected. New York Times health writer Roni Rabin made the case in a November 30, 2020, article that prisoners are being left behind despite being at high risk for Covid infection. Rabin wrote:
They live in crowded conditions, sharing bathrooms and eating facilities where social distancing is impossible. They have high rates of asthma, diabetes, and heart disease.
Many struggle with mental illness. A disproportionate number are Black and Hispanic, members of minority communities that have been hard hit by the coronavirus pandemic.
So should prisoners and other detainees be given priority access to one of the new Covid-19 vaccines?.... Yet the CDC advisory committee has prioritized correctional officers and others who work in jails and prisons for the first phase of immunizations….
Now several groups, including the American Medical Association, are calling for coronavirus vaccines to be given to inmates and employees at prisons, jails, and detention centers, citing the unique risks to people in confinement — and the potential for outbreaks to spread from correctional centers, straining community hospitals.
“We aren’t saying that prisoners should be treated any better than anybody else, but they shouldn’t be treated any worse than anybody else who is forced to live in a congregate setting,” said Dr. Eric Toner, co-author of a report on vaccine allocation published by the Johns Hopkins Center for Health Security….
Incarcerated individuals are four times more likely to become infected than people in the general population, according to a study by the criminal justice commission. Overall, Covid-19 mortality rates among prisoners are higher than in the general population.
Despite ethical and public health arguments in favor of vaccinating prisoners, CNBC News has reported that “health experts and advocates alike are deeply concerned about the notable absence of prison populations in inoculation plans.”
DeAnna Hoskins, president and CEO of JustLeadershipUSA, a national justice reform organization that seeks to cut the U.S. correctional population in half, told CNBC News that incarcerated individuals are “still considered less than human … and we are responding in that way as well when we start talking about access to vaccines.”
In the end, decisions about what groups receive top priority for vaccination reflect not only medical and scientific judgments, but also ethical and political ones, challenging us to ask hard questions about the values we hold as a society.
For Discussion:
- How much of the material in this reading was new to you, and how much was already familiar? Do you have any questions about what you read?
- What groups are likely to be first in line to receive the vaccine? What groups might be neglected?
- According to the reading, why might we prioritize prisoners as a group to receive the vaccine?
- What values or ethical considerations do you think should be taken into account by public officials as they determine what groups receive the vaccine earliest? Explain your reasoning.
Research assistance provided by Akin Olla.